Ask Doc: Why All Ankle Sprains Are Not Equal
Doc Rader 09.14.16
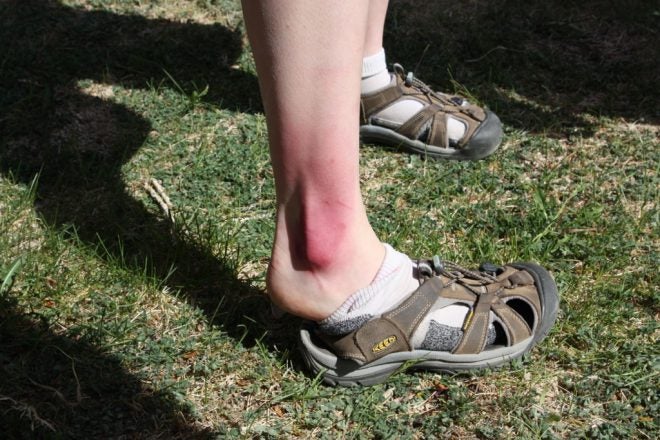
This post is not based on a question, so much as it is a public service announcement.
The weather is nice out here at this time of year, and a lot of my people are out and about enjoying the myriad of trails in the mountains and near the river. Occasionally, these trails possess annoying little rolling rocks. Or holes. Or slick wet wood. Any of which can cause a person to trip or stumble. And sometimes a bad trip or stumble can introduce a strain or sprain.
Why is this an issue? Well, most of the time it is just a soft tissue injury (muscles, tendons, ligaments). Sometimes, however, it is a bone injury. Soft tissue is generally going to heal itself, and function of the joint will be restored. A bone injury is either a surgical event, meaning you are going to need to go under the knife for a fix, or an immobilizing cast.
The problem is that the general pain related to the event is not going to tell you which type of injury you likely have. And you can likely continue to use the joint (albeit with discomfort) with either type of injury.
The issue is that if you have an avulsion fracture that is not completed (the tendon has torn the bone a little bit, but not fully detached the section), further movement can complete that tear, which will require surgery to fix. If you can immobilize it while the bone is still attached, you may be able to get away with just a cast. If the bone is fully detached you’ll want to immobilize in any case.
You need to run a test to narrow it down and determine if you should immobilize the ankle to prevent further damage (with the caveat that only radiological imagery is definitive; e.g. an X-Ray). Fortunately we have such a tool in a nice field expedient format. It is called the Ottowa Ankle Exam (which is really a set of rules developed by some emergency department doctors in, you guessed it, Ottowa, Canada back in the early 1990s).
The test is really simple, and a failure at any point means you should immobilize the ankle and go get an X-Ray. We are basically checking to see if the patient can bear weight and is free of pain, specifically “point tenderness” (think of the pain of touching a burning match to the area; basically a sharp, very specific pain, not a general ache or soreness). You test “point tenderness” using the tip of your finger, and applying pressure to the area you want to test.
![By Anatomist90 (Own work) [CC BY-SA 3.0 (http://creativecommons.org/licenses/by-sa/3.0)], via Wikimedia Commons; I added in the red circles to indicate the test areas](https://www.alloutdoor.com/wp-content/uploads/2016/09/ankle.jpg)
- Can the patient bear weight and walk on the affected ankle (don’t go more than 4 steps)
- Is there “point tenderness” to the Navicular Bone (the top of the arch of your foot)
- Is there “point tenderness” to the rear of the 5th metatarsal (like in the below video)
- Is there “point tenderness” to the rear and/or bottom of the lateral malleolus (the bottom of the long bone on the outside of your leg)
- Is there “point tenderness” to the rear and/or bottom of the medial malleolus (the bottom of the long bone on the inside of your leg)
This video is illustrative of the type of injury that is occurring (with respect to the avulsion of the 5th metatarsal). The same basic thing can happen to the ends of the tibia and fibula (the lateral and medial malleolus).
This is a very simple test you can do, and it doesn’t take a lot of time or extensive knowledge. If the subject can’t bear weight or it hurts when you touch specific areas, then it is worth it to go see a doctor and get an X-Ray.
Keep in mind if they don’t have pain (or can bear weight) they can still have a more serious injury; findings using the Ottowa Ankle Exam mean it is better to be safe than sorry.
Mandatory Disclaimer (so none of you run off and start pretending to be medics): This article is not a replacement for actually receiving training. It is for your own personal knowledge and is based on best practices and standards of training.
If you have a burning question about a wilderness medicine related concept, feel free to send an email to docrader.tfb@gmail.com. I will pick a question (or two) each week to discuss. You can read about my background below.